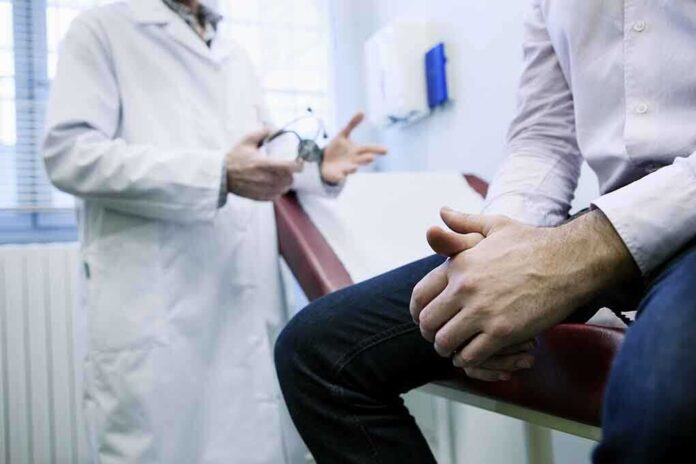
When insurance companies and hospitals clash over contract terms, patients become unwitting casualties in a financial battlefield that can leave them scrambling for care or facing crushing medical bills overnight.
Story Overview
- Contract disputes between insurers and hospitals frequently result in entire medical networks being dropped from coverage
- Patients caught in these disputes face immediate disruption to ongoing treatments and relationships with trusted physicians
- Emergency situations require immediate action to avoid unexpected out-of-network charges that can reach tens of thousands of dollars
- Strategic planning and documentation can protect patients from financial devastation during network transitions
The Insurance Network Shell Game
Healthcare networks operate like exclusive clubs where membership depends on financial negotiations between insurance companies and medical providers. When these negotiations break down, patients discover their trusted doctors have suddenly become financially toxic overnight. The timing rarely favors patients, often occurring mid-treatment or during critical care periods when switching providers poses significant medical risks.
Emergency Protocol When Your Doctor Disappears
Time becomes your enemy when network changes take effect. Contact your insurance company immediately to understand your new coverage boundaries and request a list of in-network providers in your area. Simultaneously, call your current doctor’s office to discuss transition options, including whether they offer cash-pay rates or payment plans that might be more affordable than out-of-network insurance rates.
Document everything during this process. Insurance representatives often provide conflicting information, and written records become crucial if disputes arise later. Request reference numbers for all calls and save emails confirming coverage details or exceptions.
Financial Survival Tactics
Your insurance policy likely contains continuity of care provisions that require coverage for ongoing treatments, even with out-of-network providers. Cancer treatments, pregnancy care, and other critical conditions often qualify for these exceptions. Push hard for these accommodations, as insurance companies rarely volunteer this information but frequently approve requests when pressed.
Consider the mathematics carefully before panicking. Sometimes paying cash rates directly to your preferred doctor costs less than fighting insurance bureaucracy while paying deductibles and co-pays to unfamiliar providers. Many physicians offer significant discounts for direct payment, eliminating insurance processing costs and delays.
Building Your Healthcare Defense Strategy
Prevention beats reaction in healthcare network management. Maintain relationships with multiple doctors within your insurance network, particularly for routine care. This redundancy protects against sudden network changes and provides alternatives when your primary physician becomes unavailable for any reason.
Research your insurance company’s network stability before choosing plans during open enrollment. Companies with histories of frequent provider disputes create ongoing risks for patients who value continuity of care. Sometimes paying higher premiums for stable networks saves money and stress long-term compared to constantly changing providers due to network disruptions.














